Breastfeeding Is Not Rocket Science

Most mothers and mothers-to-be have heard at some stage that 'breast is best', and that breast milk provides all the energy and nutrients that a baby needs for the first few months of their life. But, despite this, only a small percentage of women are still exclusively breastfeeding at five to six months.
So why do so many mothers stop breastfeeding their babies and switch to formula when they are not only aware of the benefits of breast milk, but that breast milk is free (and so much more convenient)?

Pic: Mother and new newborn baby breastfeeding during the first 72 hours
Ask a dozen new mothers and you’ll get 13 different answers, but the bottom line is this: while breastfeeding isn’t rocket science, it’s not always easy and far too many breastfeeding women experience pain and, crucially, a lack of support, particularly in those early postpartum days and weeks. For the simple fact is that so many new mothers are shown ‘how to breastfeed’ using commonly taught forceful techniques in the hustle and bustle of the busy hospital system.
In this blog, we’ll be looking at why many women reluctantly call time on breastfeeding, and where you can seek help if you are worried about breastfeeding and/or you have previously struggled to breastfeed but hope to avoid complications next time around.
Nipple Trauma
Painful, cracked, grazed or bleeding nipples are, rather worryingly, far too common when breastfeeding. The highly sensitive nipple tissue may feel tender, may sting and for some women, the pain can become so excruciating that they feel forced to stop breastfeeding early on.
Pic: An example of nipple trauma and areola damage - courtesy of Dr Robyn Thompson's PhD Research, 2014
It’s important to know that breastfeeding does not have to be painful. When a baby is held by the back of the head, neck or shoulders and forced to the breast, it’s highly likely that the end result will be painful nipple trauma. This technique known as the cross-cradle technique is statistically significant in relation to nipple trauma according to the PhD research of Dr Robyn Thompson, experienced midwife and breastfeeding specialist.

Pic: The commonly taught forceful technique known as the Cross-Cradle Technique
Our message? If you’re currently experiencing nipple trauma, you are encouraged to avoid the cross cradle technique. Gently cradle your baby in your arms with elbows relaxed by your side, guiding your baby gently towards your breast observing your baby’s ‘lips over your nipple’ (not ‘nipple to nose’ like commonly taught in hospitals).
Sometimes the most gentle of adjustments can make a world of difference.
And if you’re pregnant and you’d like to avoid nipple trauma (which would be the case for most women - particularly those who have struggled with nipple pain in the past), please avoid the cross cradle technique and equally important, do not let anyone touch your breasts or hold your baby by the back of the head, neck or shoulders to force your baby to your breast.
Breast Engorgement
As your breast milk production gradually increases following the 3 Golden Hours and over the first 72 - 96 hours, it’s normal for your breasts to start to feel full. This is a sign that your breast milk volume is starting to peak (also known as your milk has ‘come in’).
Over these first few days, it’s important that your healthy baby is feeding small amounts frequently alternating breasts. This process is important for hormone stimulation to create the milk producing hormones oxytocin and prolactin. Imagine your newborn baby’s stomach being close to the size of its tiny closed fist, which is why it’s necessary to be feeding small amounts frequently. This necessary process also keeps your breast milk moving through the ductal networks of your breasts, reducing the risk of breast engorgement.
If this time is interrupted or delayed and your milk is not moving through your breasts, your breasts can become overfull and breast engorgement can occur, which can be very uncomfortable and also increases the risk of mastitis.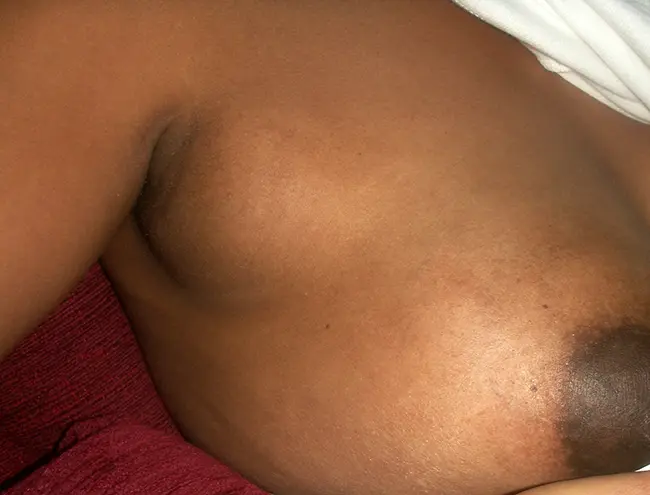
Pic: A woman with breast engorgement where milk has become congested in the 'tail of spence' - courtesy of Dr Robyn Thompson's PhD research
Some common reasons for this important mother baby time to be interrupted or delayed include:
- Unnecessary routine procedures such as weighing, checking or injecting the newborn baby.
- Hospital policies that place pressure on hospital staff to rapidly process women in, through and out of the system to early discharge
- Caesarean section, which often delays the unity of mother and baby
- A sleepy baby having difficulty staying awake to feed, associated with opiate pain administration during labour (epidural) or Caesarean Section
- Introduction of non-human milk (formula), often based on a fear of newborn weight loss
If you are well and your baby’s Apgar Score is 7 or above, your baby belongs with you.
To reduce the risk of breast engorgement (as mentioned above) it’s preferable that you have your baby with you breastfeeding frequently, alternating breasts.
If you are separated from your baby (ie NICU or Special Care Nursery), it can be a difficult time - both physically and emotionally. To reduce the risk of breast engorgement, it’s important that you gently express your breasts to ‘simulate’ what your baby would be doing under normal circumstances.
Understanding the principles of breast milk production is particularly important over this time.
Mastitis
Mastitis, otherwise known as an inflammation of the breast, is typically caused by congestion in the ductal networks and/or a blocked milk duct resulting in swollen, hot, and red breasts. It’s not uncommon for breast engorgement to develop into mastitis if not addressed early on.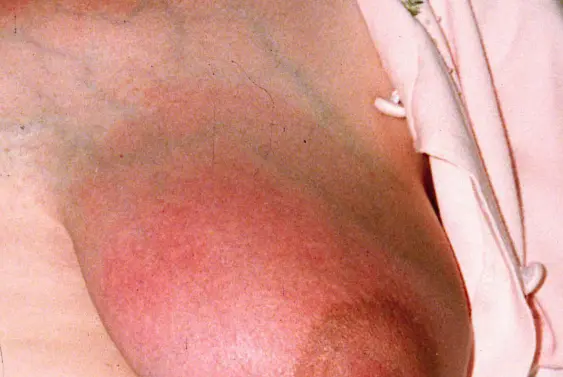
Pic: Inflamed, red area of the breast indicating mastitis - courtesy of Dr Robyn Thompson's PhD research
Other signs and symptoms of mastitis include flu-like symptoms such as fever, fatigue, and aches. Some women report a burning sensation while breastfeeding.
It’s so important to act quickly if signs of mastitis become evident, to avoid further complications. Please seek help from your midwife or other trusted healthcare professional.
The Fear of Low Milk Supply
When you first start breastfeeding, it’s not uncommon to wonder if your baby is getting enough milk. In most cases where your baby’s Apgar Score was 7 or above, and you have had an uncomplicated labour and birth, it is more than likely that you will be producing enough milk. However, pressure from the hospital system for babies to conform to specific weights and measurements can suppress a mother’s innate ability and instincts to breastfeed, creating doubt and fear.
Of course, it’s important to be reasonable in any situation where the wellbeing of a mother and her baby is concerned.
Based on the principles of human breast milk production, Dr Robyn suggests that it’s normal for your breast milk volume to be low to start with. Remember, your baby is only taking small amounts, alternating breasts, over the first few days, providing the necessary calories for your baby to feed to gastric satisfaction.
The regular, rhythmical stimulation from your baby feeding frequently, alternating breasts, increases the breast milk producing hormones oxytocin and prolactin, which in turn gradually increases your breast milk volume. The key word is ‘gradually’. This is why it’s preferable that a mother is skin to skin with her baby as much as possible over the first few days and weeks.
Pic: Newborn baby feeding frequently in the first 72 - 96 hours
Avoiding the unnecessary introduction of bottles, teats and nipple shields
It’s preferable to avoid the unnecessary introduction of non-human milk (formula) as this complicates breastfeeding. Oral devices such as bottles, teats, dummies/pacifiers and nipple shields also complicate breastfeeding as the newborn needs to adjust to the fixed silicone item. According to Dr Robyn’s experience, this may result in a brain imprint for the newborn, making the transition between device and breastfeeding complicated. 
It’s important to acknowledge that there may be times when the introduction of formula and oral devices may be of benefit to a mother and her baby. This information is shared for the purpose of bringing awareness to the potential implications for those women who would like to breastfeed.
Outdated Breastfeeding Techniques
Advice from hospital staff may be well-meaning but is often conflicting. One person often has a different opinion to the next, and so on. This can be confusing and can become quite overwhelming, particularly when you have your newborn baby in your arms. Breastfeeding techniques taught in many hospitals are often forceful, inconsistent and outdated.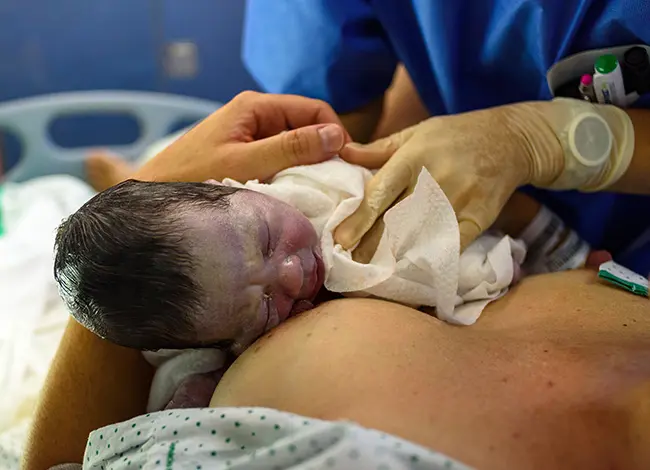
Pic: Forceful breastfeeding techniques taught in many hospitals
Dr Robyn Thompson, with 50 years of midwifery experience, both in the hospital system and with women who chose to give birth at home, observed breastfeeding complications with women discharged from hospital that she was not observing with the women who gave birth at home.
Put simply: your baby should never be forced to your breast. It’s unnecessary and impedes you and your baby’s innate instincts to develop a gentle breastfeeding rhythm that’s unique to you. Holding your baby by the back of the head, neck or shoulders, and forcing your baby to your breast significantly increases the risk of painful nipple trauma.
Where and When to Seek Breastfeeding Support
Many mothers who feel forced to discontinue breastfeeding share stories of feeling unsupported, overwhelmed, coerced by hospital policies - not to mention pain.
Please don’t wait until you give birth to learn about preparing for breastfeeding. With the right information, you will have the knowledge and confidence to create a unique birth plan that includes breastfeeding. Of course, there’s no guarantee that everything will go to plan, but with knowledge comes confidence, which means you'll be more likely to tune into and trust your maternal instincts.
The best time to begin preparing for breastfeeding is before you give birth to your baby. The Thompson Method Online Breastfeeding program is designed to help pregnant women prepare to breastfeed for as long as they choose, confidence-full and pain-free.
That being said, if you are already breastfeeding and experiencing complications, you can still turn to The Thompson Method – a gentle, evidence-based approach to breastfeeding. With lifetime access to the education and 24/7 guidance and support available in our private Facebook community, you’ll feel nurtured and supported as you work towards finding the solution to your challenges.
Dr Robyn has had the privilege to help thousands of mothers breastfeed their babies – and through her online program, she’d love to help you too.
Wondering how The Thompson Method has changed the breastfeeding journey for other women? You can read their stories here. It's a space filled with support, triumphs, and raw honesty.
To your breastfeeding journey ❤️





